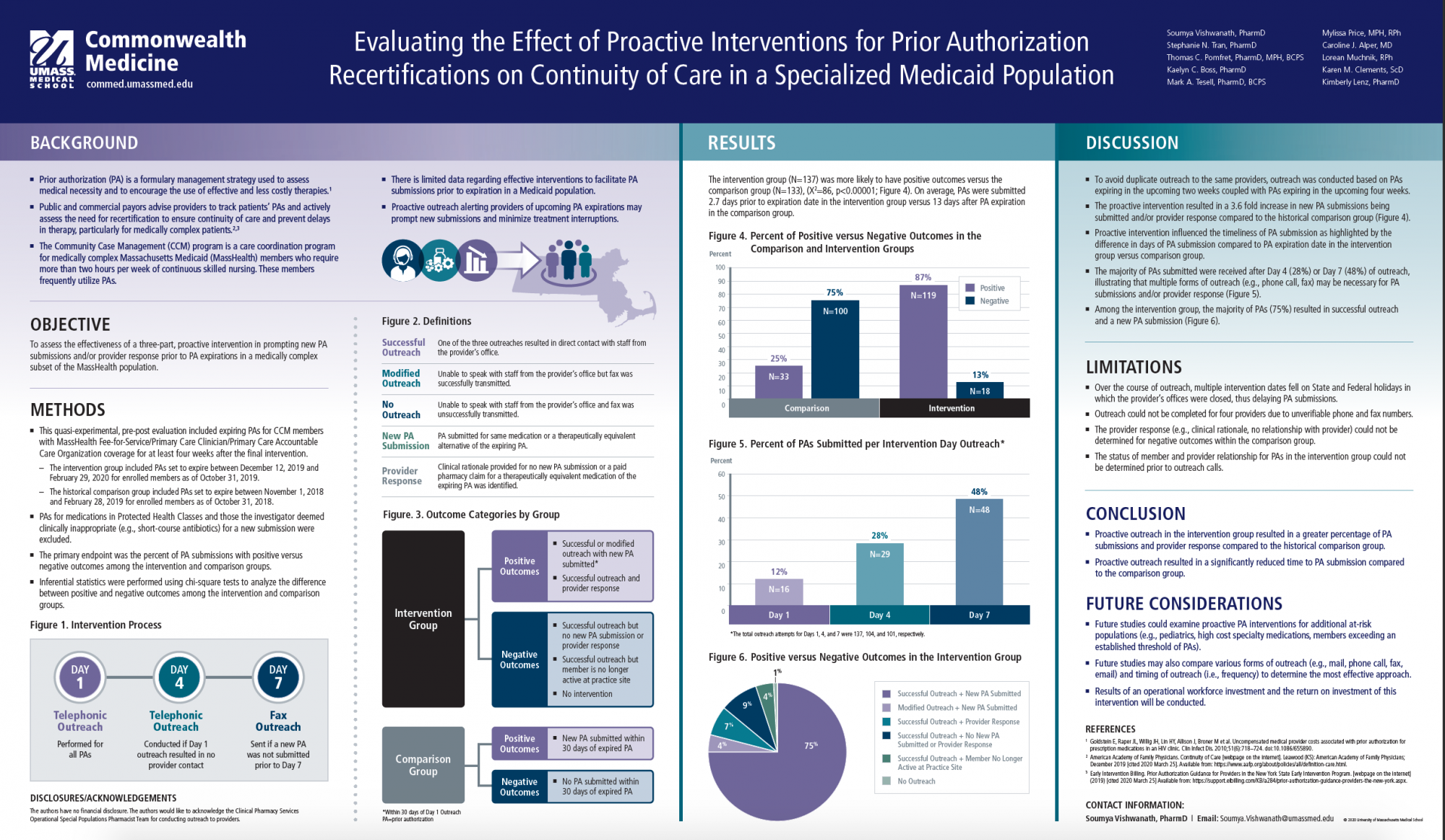
Prior authorization (PA) is a formulary management strategy used to assess medical necessity and to encourage the use of effective and less costly therapies. This study assessed the effectiveness of a three-part, proactive intervention in prompting new PA submissions and/or provider response prior to PA expiration in a medically complex subset of a state Medicaid population. Outreach in the intervention resulted in a 3.6 fold increase in new PA submissions and/or provider response compared to a historical comparison group. On average, PAs were submitted 2.7 days prior to the expiration date in the intervention group versus 13 days after PA expiration in the comparison group, highlighting the influence of the proactive intervention on the timeliness of PA submission.
Poster
Evaluating the Effect of Proactive Interventions for Prior Authorization Recertifications on Continuity of Care in a Specialized Medicaid Population
Commonwealth Medicine is now ForHealth Consulting at UMass Chan Medical School. More information available here. This content has not been updated with the new name.